BAM Chapter 14: Bacillus cereus
Bacteriological Analytical Manual (BAM) Main Page
Authors: Sandra M. Tallent, Ann Knolhoff, E. Jeffery Rhodehamel (ret.), Stanley M. Harmon (ret.), and Reginald W. Bennett (ret.)
Revision History:
October 2020: Minor Edits in Sections G and H.
November 2019: Section H.8. Addition of link to protocol for quantitative analysis for cereulide in food products.
January 2012: The Bacillus Chapter has been updated with the inclusion of a new optional chromogenic agar, Bacara agar, for the detection and enumeration of Bacillus cereus in foods.
Bacillus cereus is an aerobic spore-forming bacterium that is commonly found in soil, on vegetables, and in many raw and processed foods. B. cereus food poisoning may occur when foods are prepared and held without adequate refrigeration for several hours before serving, with B. cereus reaching >106 cells/g. Foods incriminated in past outbreaks include cooked meat and vegetables, boiled or fried rice, vanilla sauce, custards, soups, and raw vegetable sprouts. Two types of illness have been attributed to the consumption of foods contaminated with B. cereus. The first and better known is characterized by abdominal pain and non-bloody diarrhea; it has an incubation period of 4-16 h following ingestion with symptoms that last for 12-24 h. The second, which is characterized by an acute attack of nausea and vomiting, occurs within 1-5 h after consumption of contaminated food; diarrhea is not a common feature in this type of illness1. The MYP agar has been the standard media for plating B. cereus, but it has little selectivity so background flora is not inhibited and can mask the presence of B. cereus. Bacara is a chromogenic selective and differential agar that promotes the growth and identification of B. cereus, but inhibits the growth of background flora. The chromogenic agar has been suggested for the enumeration of B. cereus group as a substitute for MYP1,2. Typical colonies will grow as pink-orange uniform colonies surrounded by a zone of precipitation. The identification would include all species from the B. cereus group: B. cereus, B. thuringiensis, B. anthracis,B. mycoides, and B. weihenstephanensis. Biochemical testing will be necessary to delineate to the species level. The Bacara media can be purchased as prepared plates or media in flasks to which two supplied reagents are added. The media has a proprietary formulation and cannot be purchased in a dehydrated form.
Examination of Foods for B. cereus
-
Sampling
If the quantity of food to be examined is large, take representative samples of 50 g each from different parts of the suspect food because contamination may be unevenly distributed. If the food is a powder or consists of small discrete particles, then it should be thoroughly mixed before taking samples.
-
Transporting and storage of samples
Transport samples promptly in insulated shipping containers with enough gel-type refrigerant to maintain them at 6°C or below. Upon receipt in the laboratory, store the samples at 4°C and analyze as soon as possible. If analysis cannot be started within 4 days after collection, freeze samples promptly and store at -20°C until examined. Thaw at room temperature and proceed with analysis as usual. Maintain frozen samples at -20°C until examined. Ship on dry ice to avoid thawing. Dehydrated foods may be stored at room temperature and shipped without refrigeration.
Enumeration and Confirmation of B. cereus in Foods
- Equipment and materials
- See Chapter 1 of FDA BAM for preparation of food homogenate
- Pipets, 1, 5, and 10 ml, graduated in 0.1 ml units
- Glass spreading rods (e.g., hockey stick) 3-4 mm diameter with 45-55 mm spreading area
- Incubators, 30 ± 2°C and 35 ± 2°C
- Colony counter
- Marking pen, black felt type
- Large and small Bunsen burners
- Wire loops, No. 24 nichrome or platinum wire, 2 mm and 3 mm id
- Vortex mixer
- Microscope, microscope slides, and cover slips
- Culture tubes, 13 × 100 mm, sterile
- Test tubes, 16 × 125 mm, or spot plate
- Bottles, 3 oz, sterile
- Anaerobic jar, BBL GasPak, with H2 + CO2 generator envelopes and catalyst
- Water bath, 45 ± 2°C (tempering agar)
- Water bath, 100 ± 2°C (melting Bacara agar prepared in flask)
- Culture tube racks
- Staining rack
- Petri dishes, sterile, 15 × 100 mm
- Media and reagents
- Bacara agar plates, chromogenic media prepared plates or flasks purchased from AES Chemunex, Cranbury, NJ.
- Mannitol-egg yolk-polymyxin (MYP) agar plates (M95)
- Egg yolk emulsion, 50% (M51)
- Trypticase soy-polymyxin broth (M158)
- Polymyxin B solutions for MYP agar (0.1%) and trypticase soy-polymyxin broth (0.15%) (see M95 and M158)
- Phenol red glucose broth (M122)
- Tyrosine agar (M170)
- Lysozyme broth (M90)
- Voges-Proskauer medium (M177)
- Nitrate broth (M108)
- Nutrient agar for B. cereus (M113)
- Motility medium (B. cereus) (M100)
- Trypticase soy-sheep blood agar (M159)
- Nitrite detection reagents (R48)
- Butterfield's phosphate-buffered dilution water (R11) sterilized in bottles to yield final volumes of 450 ± 5 ml and 90 ± 2 ml
- Voges-Proskauer test reagents (R89)
- Creatine crystals
- Gram stain reagents (R32)
- Basic fuchsin staining solution (R3)
- Methanol (absolute)
- Brain Heart Infusion Broth with 0.1% glucose for enterotoxin testing (Ch. 15).
-
Sample preparation
Using aseptic technique, weigh 50 g of sample into sterile blender jar. Add 450 mL Butterfield's phosphate-buffered dilution water (1:10 dilution) and blend for 2 min at high speed (10,000-12,000 rpm). Prepare serial dilutions from 10-2 to 10-6 by transferring 10 mL homogenized sample (1:10 dilution) to 90 mL dilution blank, mixing well with vigorous shaking, and continuing until 10-6 dilution is reached.
-
Plate count of B. cereus
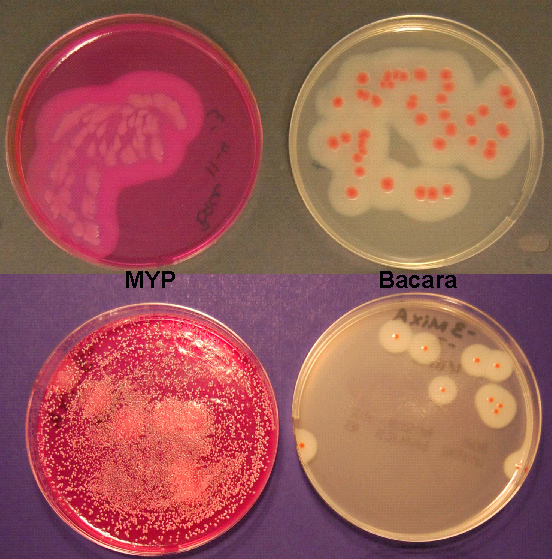
Inoculate duplicate Bacara or MYP agar plates with each dilution of sample (including 1:10) by spreading 0.1 mL evenly onto surface of each plate with sterile glass spreading rod. Incubate plates 18-24 h at 30°C and observe for colonies surrounded by precipitate zone, which indicates that lecithinase is produced. B. cereus colonies are usually a pink-orange color on Bacara or pink on MYP and may become more intense after additional incubation (see Fig. 1).
Fig. 1. Colonies of B. cereus grown on MYP are pink and lecithinase positive, but other bacteria are not inhibited and can interfere with isolation of B. cereus. Colonies of B. cereus grown on Bacara are pink-orange and are lecithinase positive, but other organisms are inhibited.If reactions are not clear, incubate plates for additional 24 h before counting colonies. Select plates that contain an estimated 15-150 pink-orange (Bacara) or pink (MYP), lecithinase-producing colonies. Mark bottom of plates into zones with black felt pen to facilitate counting and count colonies that are typical of B. cereus. This is the presumptive plate count of B. cereus. Pick at least 5 presumptive positive colonies from the Bacara or MYP plates and transfer one colony to BHI with 0.1% glucose for enterotoxin studies (Chapter 15) and a nutrient agar slant for storage. Typical colonies grown on Bacara or MYP must be confirmed with biochemical testing as described in Sections F and H below.
Calculate number of B. cereus cells/g of sample, based on percentage of colonies that are morphologically consistent with B. cereus. For example, if average count obtained with 10-4 dilution of sample was 65 and 4 of 5 colonies tested were confirmed as B. cereus, the number of B. cereus cells/g of food is 65 × 4/5 × 10,000 × 10 = 5,200,000. (NOTE: Dilution factor is tenfold higher than sample dilution because only 0.1 mL was tested).
-
Most probable number (MPN) of B. cereus
The most probable number (MPN) method is recommended for routine surveillance of products in which small numbers of B. cereus are expected5. This method is also effective in testing foods that may contain a large population of competing species or in dehydrated food products in which the potential spores would outnumber vegetative cells and require additional nutrients to germinate.
Inoculate 3-tube MPN series in trypticase soy-polymyxin broth, using 1 mL inoculum of 10-1, 10-2, and 10-3 dilutions of sample with 3 tubes at each dilution. (Additional dilutions should also be tested if B. cereus population is expected to exceed 103/g.) Incubate tubes 48 ± 2 h at 30 + 2°C and observe for turbid growth, which is typical of B. cereus. Streak cultures from turbid, positive tubes onto separate agar plates (either Bacara or MYP) and incubate plates 18-24 h at 30°C. Pick one or more pink-orange (Bacara) or pink (MYP), lecithinase-positive colonies from each agar plate and transfer to BHI with 0.1% glucose for enterotoxin studies (Chapter 15) and nutrient agar slants for storage. Typical colonies grown on Bacara or MYP must be confirmed with biochemical testing as described in Sections F and G below.
Calculate MPN of B. cereus cells/g of sample (see BAM Appendix 2) based on the number of tubes at each dilution in which the presence of B. cereus was confirmed. Biochemical testing will be necessary to delineate to the species level, however, enterotoxins can be carried by Bacillus spp. other than B. cereus.
-
Confirmation of B. cereus
Pick 5 or more eosin pink, lecithinase-positive colonies from MYP agar plates and transfer to nutrient agar slants. Incubate slants 24 h at 30°C. Prepare Gram-stained smears from slants and examine microscopically. B. cereus will appear as large Gram-positive bacilli in short-to-long chains; spores are ellipsoidal, central to subterminal, and do not swell the sporangium. Transfer 3 mm loopful of culture from each slant to 13 × 100 mm tube containing 0.5 ml of sterile phosphate-buffered dilution water and suspend culture in diluent with Vortex mixer. Use suspended cultures including ATCC 14579 B. cereus and ATCC 64 Brevibacillus laterosporus as positive and negative controls respectively to inoculate the following confirmatory media:
- Phenol red glucose broth. Inoculate 3 mL broth with 2 mm loopful of culture. Incubate tubes anaerobically 24 h at 35°C in GasPak anaerobic jar. Shake tubes vigorously and observe for growth as indicated by increased turbidity and color change from red to yellow, which indicates that acid has been produced anaerobically from glucose. A partial color change from red to orange/yellow may occur, even in uninoculated control tubes, due to a pH reduction upon exposure of media to CO2 formed in GasPak anaerobic jars.
- Nitrate broth. Inoculate 5 ml broth with 3 mm loopful of culture. Incubate tubes 24 h at 35°C. To test for nitrite, add 0.25 ml each of nitrite test reagents A and C to each culture. An orange color, which develops within 10 min, indicates that nitrate has been reduced to nitrite.
- Modified VP medium. Inoculate 5 ml medium with 3 mm loopful of culture and incubate tubes 48 ± 2 h at 35°C. Test for production of acetylmethyl-carbinol by pipetting 1 ml culture into 16 × 125 mm test tube and adding 0.6 ml alpha-naphthol solution (R89) and 0.2 ml 40% potassium hydroxide (R89). Shake, and add a few crystals of creatine. Observe results after holding for 1 h at room temperature. Test is positive if pink or violet color develops.
- Tyrosine agar. Inoculate entire surface of tyrosine agar slant with 3 mm loopful of culture. Incubate slants 48 h at 35°C. Observe for clearing of medium near growth, which indicates that tyrosine has been decomposed. Examine negative slants for obvious signs of growth, and incubate for a total of 7 days before considering as negative.
- Lysozyme broth. Inoculate 2.5 ml of nutrient broth containing 0.001% lysozyme with 2 mm loopful of culture. Also inoculate 2.5 ml of plain nutrient broth as positive control. Incubate tubes 24 h at 35°C. Examine for growth in lysozyme broth and in nutrient broth control. Incubate negative tubes for additional 24 h before discarding.
- MYP agar. This test may be omitted if primary inoculation media was Bacara or test results were clear-cut with original MYP agar plates and there was no interference from other microorganisms.. Mark bottom of a plate into six equal sections with felt marking pen, and label each section with sample number. Inoculate premarked 4 cm sq area of MYP agar plate by gently touching surface of agar with 2 mm loopful of culture. Allow inoculum to be fully absorbed before incubating for 24 h at 30°C. Check plates for lecithinase production as indicated by zone of precipitation surrounding growth. Mannitol is not fermented by isolate if growth and surrounding medium are eosin pink. (Yellow color indicates that acid is produced from mannitol.) B. cereus colonies are usually lecithinase-positive and mannitol-negative on MYP agar.
-
Record results obtained with the different confirmatory tests. Tentatively identify as B. cereus those isolates which 1) produce large Gram-positive rods with spores that do not swell the sporangium; 2) produce lecithinase and do not ferment mannitol on MYP agar; 3) grow and produce acid from glucose anaerobically; 4) reduce nitrate to nitrite (a few strains may be negative); 5) produce acetylmethylcarbinol (VP-positive); 6) decompose L-tyrosine; and 7) grow in the presence of 0.001% lysozyme.
These basic characteristics are shared with other members of the B. cereus group, including the rhizoid strains B. mycoides, the crystalliferous insect pathogen B. thuringiensis, and the mammalian pathogen B. anthracis. However, these species can usually be differentiated from B. cereus by determining specific characteristics typical of each species or variety. The tests described in H, below, are useful for this purpose and can easily be performed in most laboratories. Strains that produce atypical results from these tests require additional analysis before they can be classified as B. cereus.
-
Tests for differentiating members of the B. cereus group (Table 1)
- The following tests are useful for differentiating typical strains of B. cereus from other members of the B. cereus group, including B. mycoides, B. thuringiensis, and B. anthracis also non-motile.
Motility test. Inoculate BC motility medium by stabbing down the center with 3 mm loopful of 24 h culture suspension. Incubate tubes 18-24 h at 30°C and examine for type of growth along stab line. Motile organisms produce diffuse growth out into the medium away from the stab. Non-motile organisms produce growth only in and along stab. Alternatively, add 0.2 mL sterile distilled water to surface of nutrient agar slant and inoculate slant with 3 mm loopful of culture suspension. Incubate slant 6-8 h at 30°C and suspend 3 mm loopful of liquid culture from base of slant in a drop of sterile water on microscope slide. Apply cover glass and examine immediately with microscope for motility. Report whether or not isolates tested were motile. Most strains of B. cereus and B. thuringiensis are motile by means of peritrichous flagella. B. anthracis and all except a few strains of B. mycoides are non-motile. A few B. cereus strains are also non-motile.
Table 1. Differential characteristics of large-celled Group I Bacillus speciesFeature B. cereus B. thuringiensis B. mycoides B. weihenstephanensis B. anthracis B. megaterium Gram reaction +(a) + + + + + Catalase + + + + + + Motility +/−(b) +/− −(c) + − +/− Reduction of nitrate + + + + + −(d) Tyrosine decomposed + + +/− + −(d) +/− Lysozyme-resistant + + + + + − Egg yolk reaction + + + + + − Anaerobic utilization of glucose + + + + + − VP reaction + + + + + − Acid produced from mannitol − − − − − + Hemolysis (Sheep RBC) + + + ND −(d) − Known pathogenicitye
/characteristicproduces enterotoxins endotoxin crystals
pathogenic to insectsrhizoidal growth growth at 6°C;
no growth at 43°Cpathogenic to animals and humans a +, 90-100% of strains are positive.
b +/−, 50-50% of strains are positive.
c −, 90-100% of strains are negative.
d −, Most strains are negative.
e See Section 7, Limitations of method for B. cereus.
ND Not determined -
Rhizoid growth. Pour 18-20 mL nutrient agar into sterile 15 × 100 mm petri dishes and allow agar to dry at room temperature for 1-2 days. Inoculate by gently touching surface of medium near center of each plate with 2 mm loopful of 24 h culture suspension. Allow inoculum to be absorbed and incubate plates 48-72 h at 30°C. Examine for development of rhizoid growth, which is characterized by production of colonies with long hair or root-like structures that may extend several centimeters from site of inoculation. Rough galaxy-shaped colonies are often produced by B. cereus strains and should not be confused with typical rhizoid growth, which is the definitive characteristic of B. mycoides. Most strains of this species are also non-motile.
-
Test for hemolytic activity. Mark bottom of a plate into 6-8 equal sections with felt marking pen, and label each section. Inoculate a premarked 4 cm sq area of trypticase soy-sheep blood agar plate by gently touching medium surface with 2 mm loopful of 24 h culture suspension. (Six or more cultures can be tested simultaneously on each plate.) Incubate plates 24 h at 35°C. Examine plates for hemolytic activity. B. cereus cultures usually are strongly hemolytic and produce 2-4 mm zone of complete (β) hemolysis surrounding growth. Most B. thuringiensis and B. mycoides strains are also β-hemolytic. B. anthracis strains are usually nonhemolytic after 24 h incubation.
-
Test for protein toxin crystals. Inoculate nutrient agar slants with 3 mm loopfuls of 24 h culture suspensions. Incubate slants 24 h at 30°C and then at room temperature 2-3 days. Prepare smears with sterile distilled water on microscope slides. Air-dry and lightly heat-fix by passing slide through flame of Bunsen burner. Place slide on staining rack and flood with methanol. Let stand 30 s, pour off methanol, and allow slide to air-dry. Return slide to staining rack and flood completely with 0.5% basic fuchsin or TB carbolfuchsin ZN stain (Difco). Heat slide gently from below with small Bunsen burner until steam is seen.
Wait 1-2 min and repeat this step. Let stand 30 s, pour off stain, and rinse slide thoroughly with clean tap water. Dry slide without blotting and examine under oil immersion for presence of free spores and darkly stained tetragonal (diamond-shaped) toxin crystals. Crystals are usually somewhat smaller than spores. Toxin crystals are usually abundant in a 3- to 4-day-old culture of B. thuringiensis but cannot be detected by the staining technique until lysis of the sporangium has occurred. Therefore, unless free spores can be seen, cultures should be held at room temperature for a few more days and re-examined for toxin crystals. B. thuringiensis usually produces protein toxin crystals that can be detected by the staining technique either as free crystals or parasporal inclusion bodies within the exosporium. B. cereus and other members of the B. cereus group do not produce protein toxin crystals.
-
Test for psychrotolerant strains. To determine psychrotolerance streak out two TSA plates. Incubate one plate at 6°C for 28 days and the second at 43°C for 4 days. B. weihenstephanensis will grow at 6°C but not at 43°C.
- Interpreting test results. On the basis of the test results, identify as B. cereus those isolates which are actively motile and strongly hemolytic and do not produce rhizoid colonies or protein toxin crystals. Nonmotile B. cereus strains are also fairly common and a few strains are weakly hemolytic. These nonpathogenic strains of B. cereus can be differentiated from B. anthracis by their resistance to penicillin and gamma bacteriophage. CAUTION: Nonmotile, nonhemolytic isolates that are suspected to be B. anthracis should be submitted to a pathology laboratory such as the Centers for Disease Control and Prevention, Atlanta, GA, for identification or destroyed by autoclaving. Acrystalliferous variants of B. thuringiensis and nonrhizoid strains derived from B. mycoides cannot be distinguished from B. cereus by the cultural tests.
-
Limitations of method for B. cereus. The method described is intended primarily for use in the routine examination of foods. As noted in F above and in Table 1, the confirmatory tests recommended may in some instances be inadequate for distinguishing B. cereus from culturally similar organisms that could occasionally be encountered in foods. These organisms include 1) the insect pathogen B. thuringiensis, which produces protein toxin crystals; 2) B. mycoides, which characteristically produces rhizoid colonies on agar media; and 3) B. anthracis, which exhibits marked animal pathogenicity and is non-motile. With the exception of B. thuringiensis, which is currently being used for insect control on food and forage crops, these organisms are seldom encountered in the routine examination of foods. The tests described above are usually adequate for distinguishing the typical strains of B. cereus from other members of the B. cereus group. However, results with atypical strains of B. cereus are quite variable, and further testing may be necessary to identify the isolates.
- Test for cereulide (emetic toxin). Intoxication is caused by the pre-formed cereulide produced by B. cereus spores after germinating in food that has not been stored properly. Ingestion of the pre-formed toxin typically begets nausea and vomiting. The cereulide is resistant to acid, heat and digestive enzymes. The cyclic dodecadepsipeptide acts as an ionophore disrupting oxidative phosphorylation in the mitochondria and has been associated with several cases of liver failure (Mahler et al. 1997; Dierick et al. 2005; Pósfay-Barbe et al. 2008). This method outlines procedures to perform quantitative analysis for cereulide, or emetic toxin, associated with some strains of Bacillus cereus. The toxin can be produced in foods contaminated with enterotoxigenic strains causing human illness. Symptoms include nausea and vomiting, but intoxication has been associated with severe illness and death.
- The following tests are useful for differentiating typical strains of B. cereus from other members of the B. cereus group, including B. mycoides, B. thuringiensis, and B. anthracis also non-motile.
References
- Stenfors, Arnesen LP, Fagerlund A, Granum PE. (2008) From Soil to gut: Bacillus cereus and its food poisoning toxins. FEMS Microbiol Rev. 32: 579-606.
- Tallent, SM, KM Kotewicz, EA Strain and RW Bennett. 2012. Efficient Isolation and Identification of Bacillus cereus Group
 . Journal of AOAC International, 95(2): 446-451. Available as PDF (278 Kb)
. Journal of AOAC International, 95(2): 446-451. Available as PDF (278 Kb) - Anonymous. (1993) 2nd Ed., International Organization for Standardization, Geneva, Switzerland, Method ISO 793.
- Mahler, H., Pasi, A., Kramer, J.M., Schulte, Pl, Scoging, A.C., Bar, W. and Krahenbuhl, L.S. (1997). (1997). Fulminant liver failure in association with the emetic toxin of Bacillus cereus. N. Engl. J. Med. 336: 1142–1148.
- Dierick, K. Van Coillie, E., Swiecicka, I., Meyfroidt, G., Devlieger, H., Meulemans, A., Hoedemaekers, G., Fopurie, L., Heyndricks, M., and Mahillon, J. (2005). Fatal family outbreak of Bacillus cereus-associated food poisoning.
- Posfay-Barbe, K.M., Schrenzel, J., Frey, J., Studer, R., Korff, C., Belli, D.C., Parvex, Pl, Rimensberger, P.C., and Schappi, M.G. (2008). Food poisoning as a cause of acute liver failure. Pediatr. Infect. Dis. J. 27: 846–847.
Hypertext Source: Bacteriological Analytical Manual, 8th Edition, Revision A, 1998. Chapter 14.